Dr Frank Scaccia at Riverside Plastic Surgery Center specilaizes in removal of all types of skin growths from most parts of the body. These growths can be either benign (noncancerous) or malignant. Benign growths include skin tags, moles, scars from previous surgery or trauma, warts, age spots, seborrheic keratosis, actinic keratosis, cherry angiomas, lipoma, sebaceous cysts, keloids, scalp cysts, vascular lesions, hyperpigmenation, spider veins, split earlobes and pyogenic granulomas. Malignant lesions include basal cell carcinoma, squamous cell carcinoma, and malignant melanoma.
Riverside treats each case individually and has all of the state of the art equipment and skills to treat each of these skin disorders with minimal discomfort, quick healing, and at time practically scarless. We have the latest model of the Ellman Radiosurgical Unit that allows certain lesions to be removed without the use of a knife and sutures. It is very precise and done with microscopic visual aid which further enhances the success of the outcome. Often lesions on certain parts of the face where previously other practioners and dermatologists are wary of removing Dr Scaccia will successfully remove. Dr Scaccia has over 20 years of experience using radio surgery for lesion removal and is a pioneer in its use for this in the NJ area. If it is deemed necessary a lesion needs to be surgically excised Dr Scaccia will perform a meticulous plastic surgery repair again under microscopic magnification to ensure a beautiful outcome. If the lesion is suspicious and needs to be sent for pathology the procedure is often covered by your insurance plan . When a know skin cancer is being removed since our office and in office surgery center is directly across the street from Riverview Meridian Medical center we can often send your lesion for same day immediate diagnosis and frozen section control just as would happen in a hospital OR setting. Then immediate decisions can be made for completing the resection and obtaining tumor free margins and skin closure. Very often lesion removal can be done on the same day of your initial appointment if time allows and you have not been taking aspirin or fish oils or advil,etc. Furthermore. Riverside has access to the latest version of Pulse Dye laser treatments for further refinements of your scar postop to ensure even more perfect results. And finally all work is done personally by Dr Scaccia as he does not employ Physician assistants or nurse practioners. He will personally follow up with you and take out his own sutures. You can trust Dr Scaccia as he is a perfectionist and has many years of experience in performing these procedures. He is a double board certified Facial Plastic Surgeon and a 2007-2015 Top NY Metro Castle Connelly award recipient.
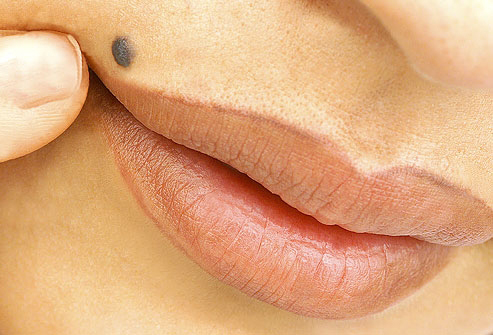
What is a Mole?
A mole (nevus) is a pigmented (colored) spot on the outer layer of the skin (epidermis).
Moles can be round, oval, flat, or raised. They can occur singly or in clusters on any part of the body. Most moles are brown, but colors can range from pinkish flesh tones to yellow, dark blue, or black.
Everyone has at least a few moles. They generally appear by the time a person is 20 and resemble freckles at first. A mole’s color and shape don’t usually change. Changes in hormone levels that occur during puberty and pregnancy can make moles larger and darker. New moles may also appear during this period.
A mole usually lasts about 50 years before beginning to fade. Some moles disappear completely, and some never lighten at all. Some moles develop stalks that raise them above the skin’s surface; these moles eventually drop off. Types of moles.
About 1-3% of all babies have one or more moles when they are born. Moles that are present at birth are called congenital nevi.
Other Types of Moles Include:
- Junctional moles, which are usually brown and may be flat or slightly raised.
- Compound moles, which are slightly raised, range in color from tan to dark brown, and involve pigment-producing cells (melanocytes)
in both the upper and lower layers of the skin (epidermis and dermis). - Dermal moles, which range from flesh-color to brown, are elevated, most common on the upper body, and may contain hairs.
- Sebaceous moles, which are produced by over-active oil glands and are yellow and rough-textured.
- Blue moles, which are slightly raised, colored by pigment deep within the skin, and most common on the head, neck, and arms of women.
Most moles are benign, but atypical moles (dysplastic nevi) may develop into malignant melanoma,
a potentially fatal form of skin cancer.
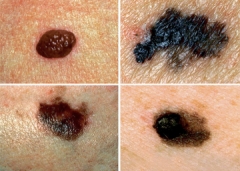
Atypical moles are usually hereditary. Most are bigger than a pencil eraser, and the shape and pigmentation are irregular.
Congenital nevi are more apt to become cancerous than moles that develop after birth, especially if they are more than eight inches in diameter.
Lentigo maligna (melanotic freckle of Hutchinson), most common on the face and after the age of 50, first appears as a flat spot containing two or more shades of tan. It gradually becomes larger and darker. One in three of these moles develop into a form of skin cancer known as lentigo maligna melanoma.
Moles are brown or black growths, usually round or oval, that can appear anywhere on the skin. They can be rough or smooth, flat or raised, single or in multiples. They occur when cells that are responsible for skin pigmentation, known as melanocytes, grow in clusters instead of being spread out across the skin. Generally, moles are less than one-quarter inch in size. Most moles appear by the age of 20, although some moles may appear later in life. Most adults have between 10 and 40 moles. Because they last about 50 years, moles may disappear by themselves over time.
Most moles are harmless, but a change in size, shape, color or texture could be indicative of a cancerous growth. Moles that have a higher-than-average chance of becoming cancerous include: Congenital Nevi
Moles present at birth. The larger their size, the greater the risk for developing into a skin cancer.
A Typical Dysplastic Nevi
Irregularly shaped moles that are larger than average.
They often appear to have dark brown centers with light, uneven borders. Higher frequency of moles.
People with 50 or more moles are at a greater risk for developing a skin cancer.
In some cases, abnormal moles may become painful, itchy, scaly or bleed. It’s important to keep an eye on your moles so that you can catch any changes early. We recommend doing a visual check of your body monthly, including all areas that don’t have sun exposure (such as the scalp, armpits or bottoms of feet).
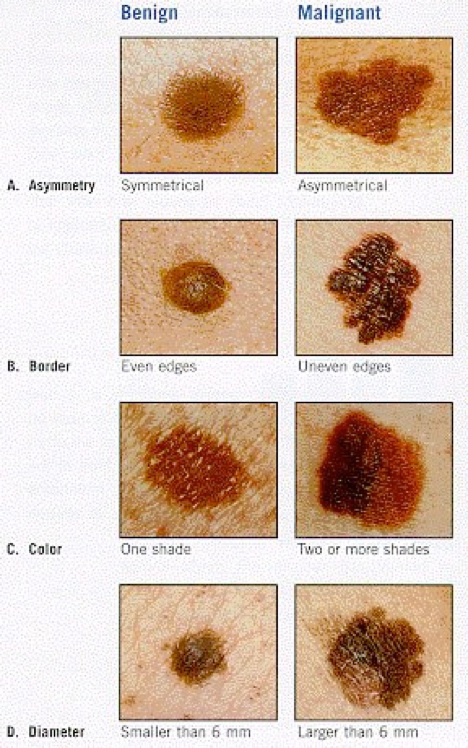
A Guide for Assessing Whether or not a Mole may be Becoming Cancerous
- Asymmetry: Half the mole does not match the other half in size, shape or color.
- Border: The edges of the mole are irregular or blurred.
- Color: The mole is not the same color throughout.
- Diameter: The mole is larger than one-quarter inch in size.
- Elevation: The mole becomes elevated or raised from the skin.
If any of these conditions occur, please make an appointment to see Dr Scaccia right away. The Dr may do a biopsy of the mole to determine if it is or isn’t cancerous and/or may surgically remove it.
Causes and Symptoms
The cause of moles is unknown, although atypical moles seem to run in families and result from exposure to sunlight.
In the past several years, researchers have identified two genes known as CDKN2A and CDK4 that govern susceptibility to melanoma in humans. Other susceptibility genes are being sought as of early 2003. Most experts, however, think that these susceptibility genes are not sufficient by themselves to account for moles becoming cancerous but are influenced by a combination of other inherited traits and environmental factors. Diagnosis
Only a small percentage of moles require medical attention. A mole that has the following symptoms should be evaluated by Dr Scaccia (a physician specializing in skin diseases).
- Appears after the age of 20
- Bleeds
- Itches
- Looks unusual or changes in any way.
If Dr Scaccia suspects skin cancer he will remove all or part of the mole for microscopic examination. This procedure, which is usually performed in the Dr’s office, is simple, relatively painless, and does not take more than a few minutes. Because Dr Scaccia utilizes his scar less technique it does not leave a scar unlike many other physician’s procedures.
Moles are rarely cancerous and, once removed, unlikely to recur. Dr Frank Scaccia should be consulted if a mole reappears after being removed.
Prevention
Wearing a sunscreen and limiting sun exposure may prevent some moles.
Anyone who has moles should examine them every month and visit Dr Scaccia if changes in size, shape, color, or texture occur or if new moles appear.
A team of researchers at Duke University where Dr Scaccia attended college and graduated Magna Cum Laude and Phi Beta Kappa reported in 2003 that topical application of a combination of 15% vitamin C and 1% vitamin E over a four-day period offered significant protection against Sun Burn.
The researchers suggest that this combination may protect skin against aging caused by sunlight as well.
Warts
A Wart is generally a small, rough growth, typically on a human’s hands or feet but often other locations, that can resemble a cauliflower or a solid blister.
They are caused by a viral infection, specifically by one of the many types of human papillomavirus.
There are as many as 10 varieties of warts, the most common considered to be mostly harmless. It is possible to get warts from others; they are contagious and usually enter the body in an area of broken skin. They typically disappear after a few months but can last for years and can recur.
Types of Warts
A range of types of wart have been identified, varying in shape and site affected, as well as the type of human papillomavirus involved.
Some common warts include:
- Common wart ( Verruca vulgaris ), a raised wart with roughened surface, most common on hands, but can grow anywhere on the body;
- Flat wart ( Verruca plana ), a small, smooth flattened wart, flesh-colored, which can occur in large numbers; most common on the face, neck, hands, wrists and knees;
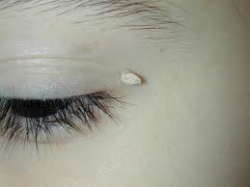
- Filiform or digitate wart, a thread- or finger-like wart, most common on the face, especially near the eyelids and lips;
- General wart (venereal wart, Condyloma acuminatum , Verruca acuminata ), a wart that occurs on the genitalia.
- Mosaic wart, a group of tightly clustered plantar-type warts, commonly on the hands or soles of the feet;
- Periungual wart a cauliflower-like cluster of warts that occurs around the nails.
- Plantar wart (verruca, Verruca plantaris ), a hard sometimes painful lump, often with multiple black specks in the center; usually only found on pressure points on the soles of the feet.
What is a Skin Tag (Acrochordon)?
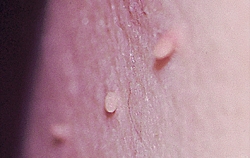
Skin tags are common, acquired, benign skin growths that look like a small piece of soft, hanging skin.
Skin tags are harmless growths. Some individuals may be more prone to tags (greater than 50-100 tags) either through increased weight, in part combined with heredity, or other unknown causes. Males and females are equally prone to developing skin tags. Obesity and being moderately overweight (even temporary increases in weight) dramatically increase the chances of having skin tags.
Women of normal weight with larger breasts are also more prone to developing skin tags under their breasts.
Some small tags spontaneously rub or fall off painlessly and the person may not even know they had a skin tag. Most tags do not fall off on their own and persist once formed. The medical name for skin tag is acrochordon.
Interested in learning more? Please contact the staff at riverside facial plastic surgery and sinus center about scheduling an appointment.

